Understanding how posting contracted fees affects Dentrix Ascend
With the No write-off. Post contracted fee, if applicable option selected (on the Ledger Rules tab of the Ledger Options page), you can have Dentrix Ascend post the contracted (max allowed) fee for a procedure in a patient's ledger or treatment plan. Having this option selected affects the following areas of Dentrix Ascend:
-
Treatment plans
-
Treatment plan previews
-
Treatment plan previews - summary and detailed views
-
Ledgers and claims
-
Fee schedules
-
Other considerations
Treatment plans
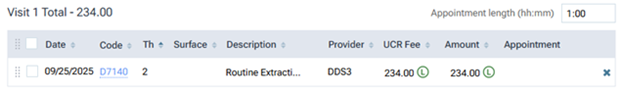
After switching to posting contracted fees, the Amount column still appears, but now a UCR Fee column also appears. Also, an orange, triangular warning icon appears in the Amount column for each procedure (and next to the visit total) because the amounts do not match the fees in the contracted fee schedule (assuming the patient has an in-network insurance plan with a Max allowable amount fee schedule selected).
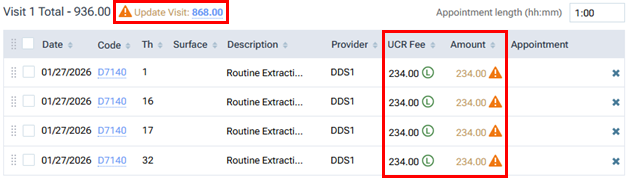
Notes:
-
The amounts in the treatment plan cannot be updated automatically to the contracted rate. It is fine if you choose not to update the amount because the write-off will still be estimated.
-
For an appointment that was scheduled previously with a procedure from a patient's treatment plan with the UCR fee, when you complete that procedure, if you do not update the amount, the procedure will be posted to the ledger with the UCR fee.
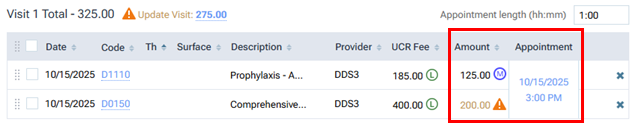
To update the Amount for each of the patient's treatment-planned procedures to be the fee from the plan's contracted fee schedule, you must do one of the following:
-
Update each procedure's amount separately.
-
Update the visit total.
With the visit total (and corresponding procedure amounts) updated, the warnings disappear.
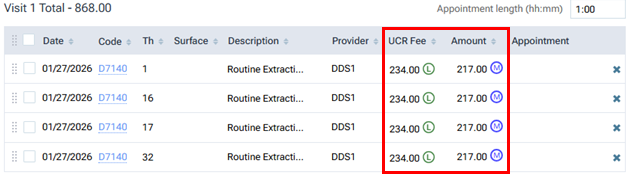
A UCR Fee comes from the fee schedule assigned to the provider associated with the procedure; or if a fee schedule is not assigned to the provider, the UCR fee comes from the fee schedule assigned to the location.
For an Amount to be the contracted fee, the patient must have insurance coverage, the billing or rendering provider (according to the location's insurance defaults—the setting to calculate contracted amounts based on billing or rendering provider, and the applicable billing or rendering provider) must be contracted with the carrier of the patient's insurance plan, and the plan must have a Max allowable amount fee schedule selected.
You can click (or tap) a blue M icon to view the name of the fee schedule that the contracted fee is coming from.
![]()
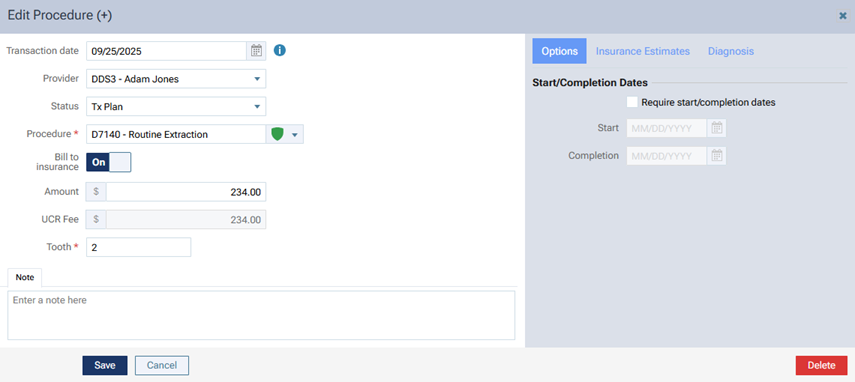
In the Edit Procedure dialog box that you open for procedure in a treatment plan, a UCR Fee box appears below the Amount box.
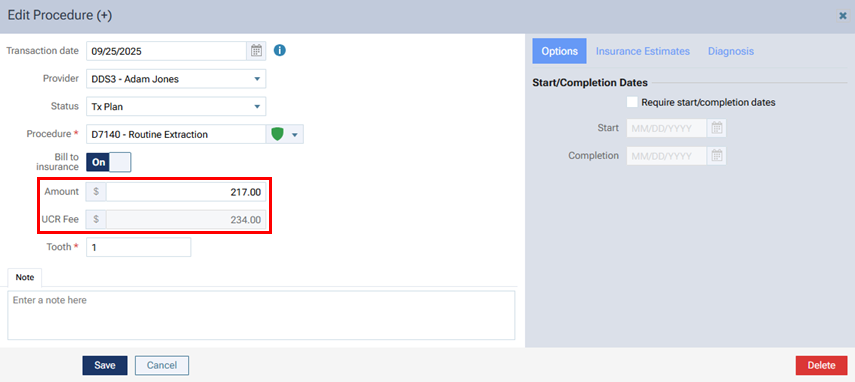
Treatment plan previews
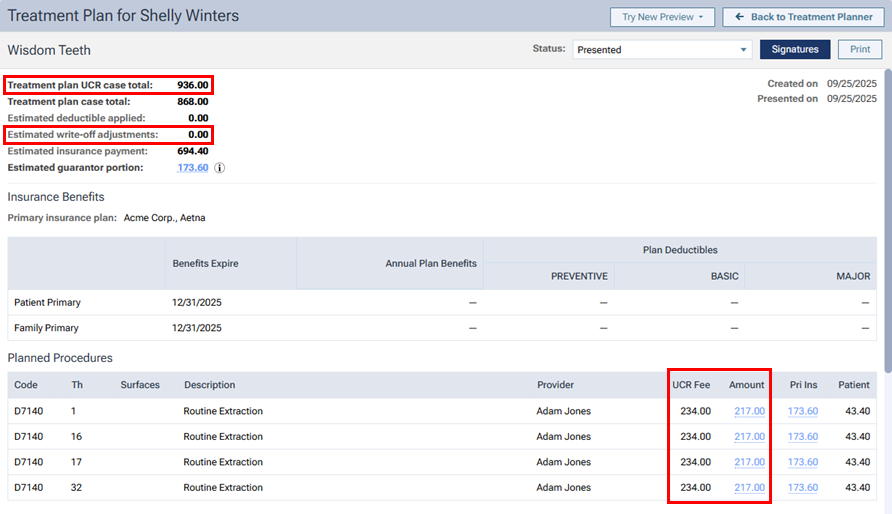
When you are presenting a treatment plan, a UCR Fee column appears next to the Amount column, a Treatment plan UCR case total appears, and a zero-dollar amount (0.00) appears for the Estimated write-off adjustments.
Treatment plan previews (enhanced)
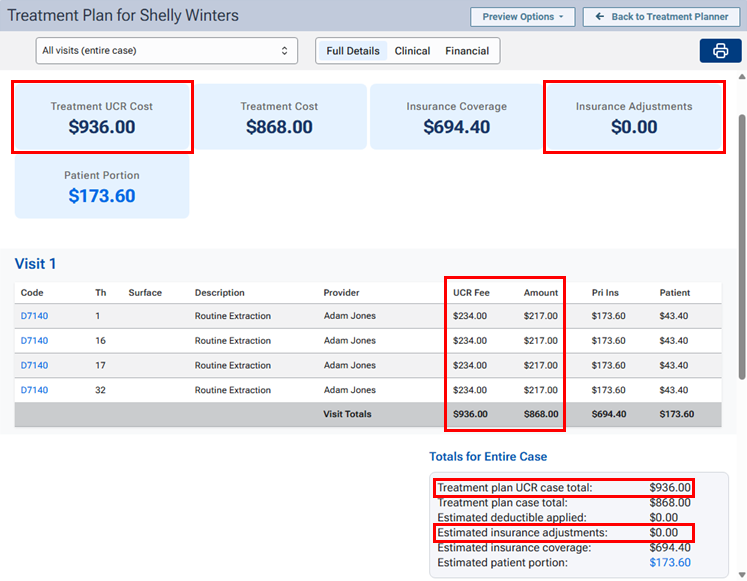
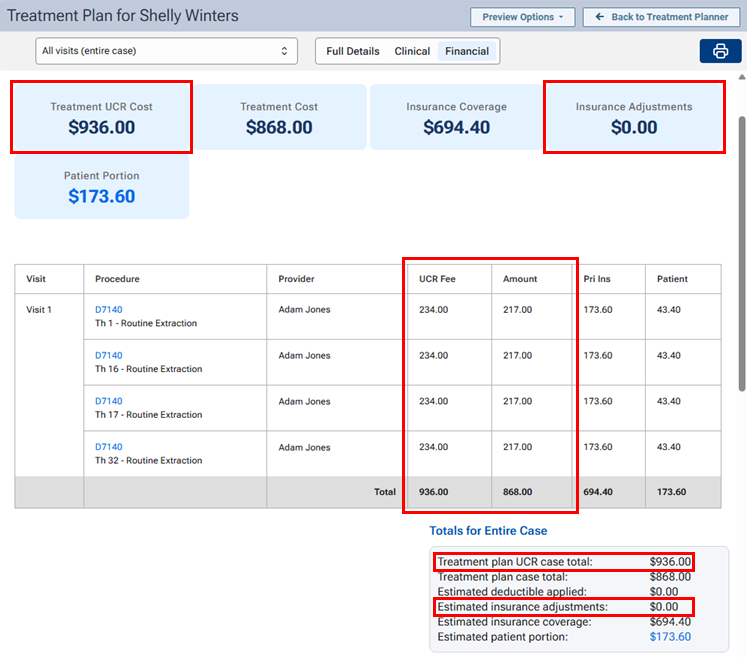
When you are presenting a treatment plan using the enhanced view, a UCR Fee column appears next to the Amount column, a Treatment UCR Cost box appears, and a zero-dollar amount (0.00) appears in the Insurance Adjustments box. Under Totals for Entire Case, a Treatment plan UCR case total appears, and a zero-dollar amount (0.00) appears for the Estimated insurance adjustments.
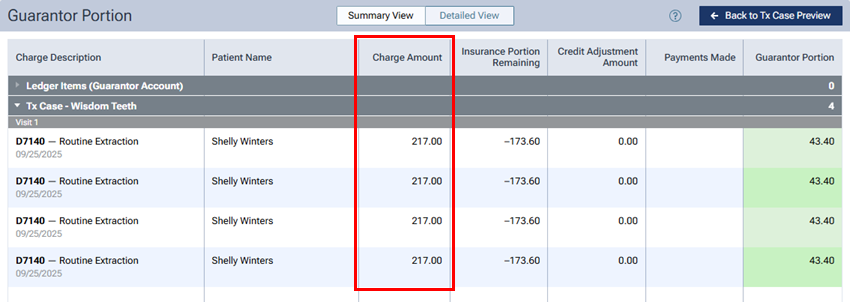
Treatment plan previews - summary and detailed views
In the Summary View and Detailed View of the treatment plan preview, the Charge Amount equals the Primary Allowable Amount if the contracted fee is posted.
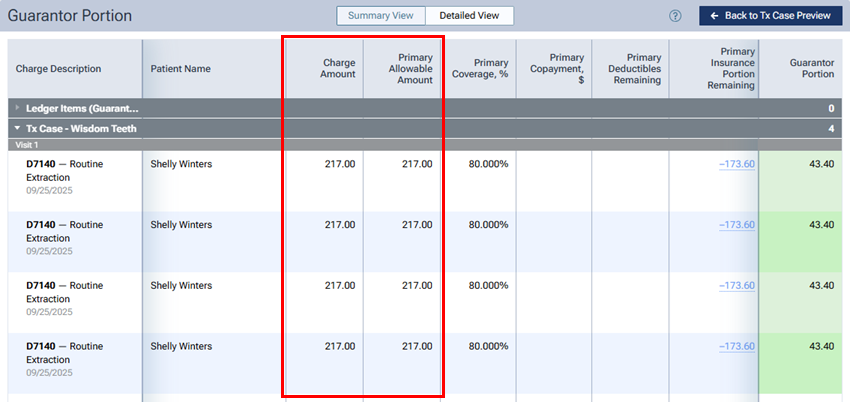
Ledgers and claims
In a patient's ledger, an indicator (orange, triangular warning icon) now appears if a procedure's amount does not match the max allowable fee schedule.
![]()
Note: This indicator appears only if the following criteria are met:
-
The No write-off. Post Contracted Fee, if applicable option is enabled.
-
The amount for the procedure has changed due to insurance, contract status, fee change, or so on.
-
The procedure was posted in the same location that you are currently logged in to.
-
A claim has not yet been created for the procedure.
-
The transaction date for the procedure is today.
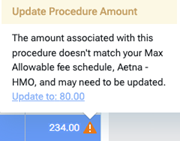
You can click the warning icon to see which max allowable fee schedule the procedure amount does not match. To update the procedure amount to match what is in the max allowable fee schedule, click the Update to [amount] link.
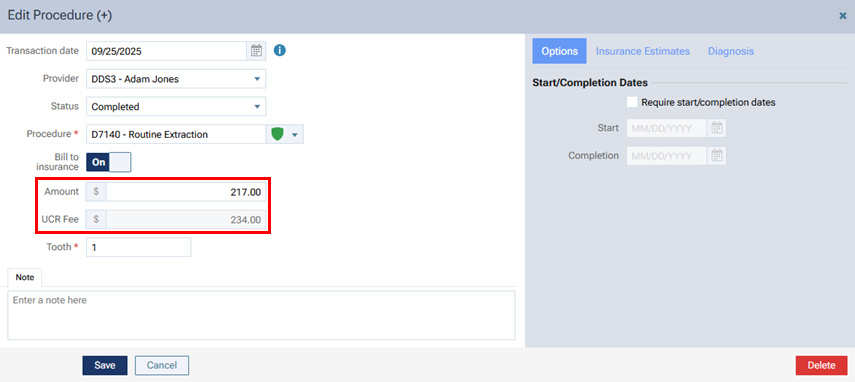
In the Edit Procedure dialog box that you open for procedure on a ledger, a UCR Fee box appears below the Amount box.
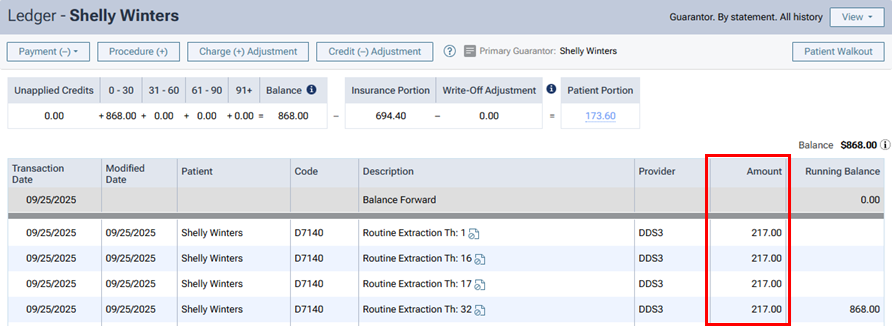
If the contracted fee was posted for a procedure, when you complete the procedure, that amount appears in the Amount column on a patient's Ledger page.
However, the UCR fees are associated with the claim throughout Dentrix Ascend (in the Patient Walkout dialog box, on the Ledger page, in the Claim Detail dialog box, on the patient's Insurance Claims page, on the Create Claims page, on the Unsent Claims page, on the Sent Claims page, on the Unresolved Claims page, and on the Outstanding Claims page).
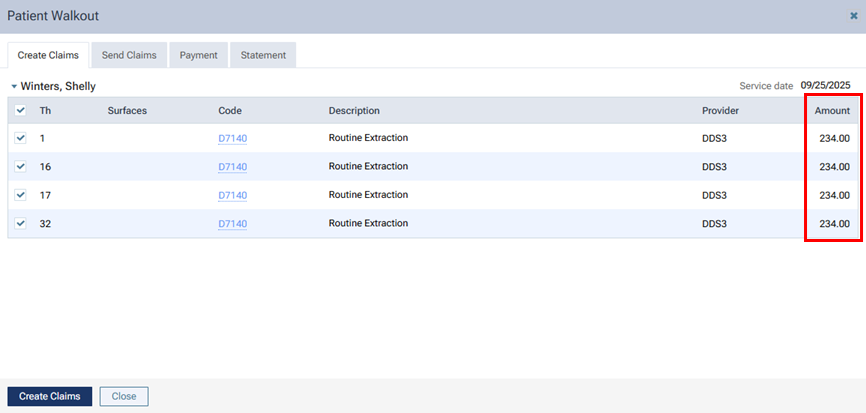
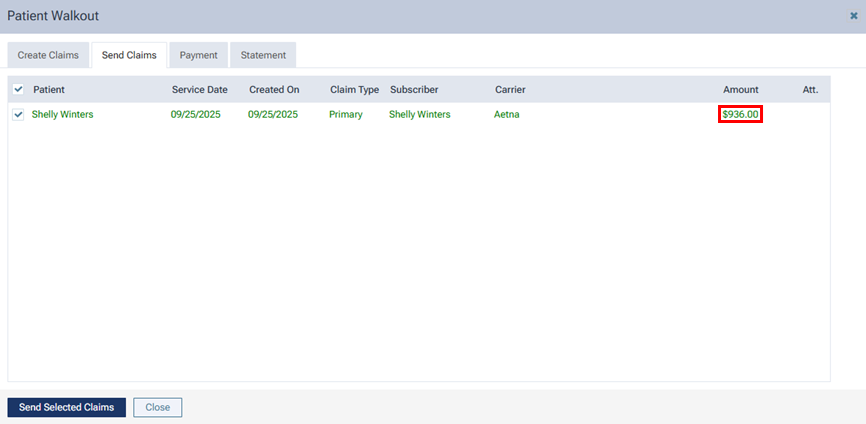
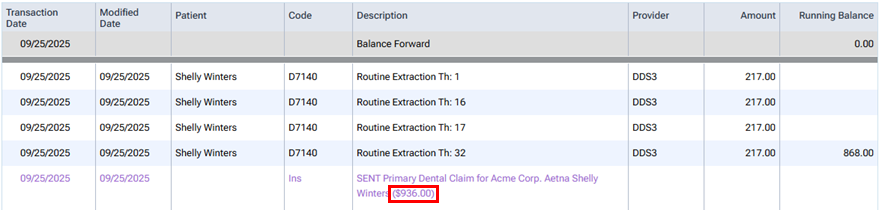
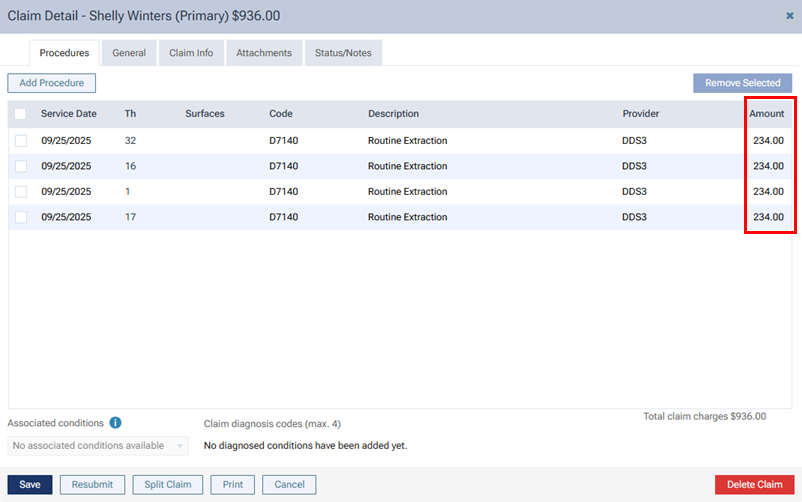
Fee schedules
For fee schedules, the No Write-off column is replaced by a Post UCR Fee column.
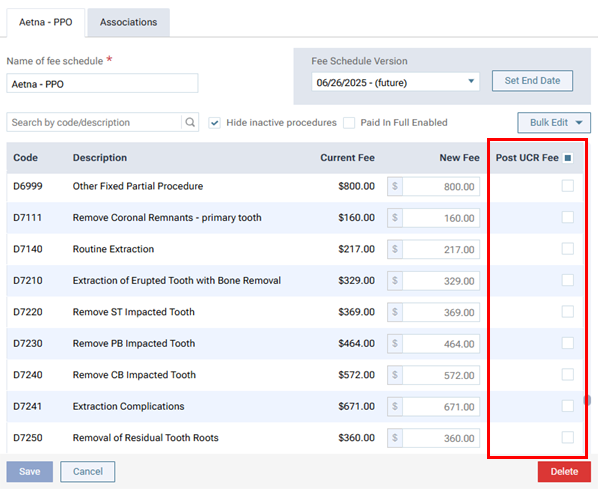
With the checkbox in the Post UCR Fee column selected for a procedure in the contracted fee schedule, when you post the procedure, the Amount comes from the UCR fee instead of the contracted fee schedule.

Other considerations
-
Generally, patient portions and overall balances should not change between your current configuration (posting a UCR fee with an insurance adjustment) versus the new configuration (posting a contracted fee without an adjustment).
-
The estimated secondary insurance portion can be an amount up to the primary plan's contracted fee.
-
For discount plans, a procedure's Amount comes from the discount/sliding fee schedule, and an adjustment is not posted. A discount plan assigned to a patient continues to apply only if the patient does not have insurance coverage.
-
The Calendar page does not display "Gross Production" because that data will be similar if not the same as the "Net Production."
-
Route slips display the contracted fee, if applicable.
-
The "Procedure Charges" on the Provider A/R Totals Report displays what was posted to the ledger (contracted fee, discount fee, or UCR fee), so you will likely see less in the "Credit Adj." columns.
-
On a day sheet, fields such as "Procedure Charges," "Estimated Net Production," "Average Production Per Patient," and "Average Charge Per Procedure" display what was posted to the ledger (contracted fee, discount fee, or UCR fee). However, "Charges Billed to Insurance" displays the UCR fee because that is what was sent on the claim to insurance.
-
Because the contracted/allowed amount becomes the amount that is charged for a procedure, there are no insurance adjustments (in theory), so you cannot use the Insurance Utilization Report to get an idea of how much you are writing off and use that information for negotiating rates with carriers. Similarly, any report you might have created that allowed you to see how much you were "giving away" with your discount plans is no longer relevant.
-
If there is an insurance overpayment—which may happen more often now for patients with secondary insurance because the primary contracted fee is being posted—follow these steps:
-
Create a new payment.
-
Post the full amount of the payment.
-
Select an offsetting insurance adjustment (using a "collection" charge adjustment).
-
Ensure that the other payment allocations by procedure are correct.
-
Save the payment.
-
For each provider to whom you want to allocate these credits, do the following:
-
Post a "production" charge adjustment for the amount to be credited to the provider's production.
-
Post a "collection" credit adjustment for the amount to be credited to the provider's production.
-
-