

When eligibility responses are returned, an eligibility icon appears automatically in the Appointment Book and the Family File based on status. Eligibility indicator icons are color-coded (and independent of the color coding of the appointment blocks in the Appointment Book designating each provider) as follows:
White E on Green Background – Patient is Eligible, and current data is already saved to the coverage tables.
![]()
Green E on White Background (with small red corner box) – Patient is eligible, and new eligibility data is ready for review and approval to be saved to the coverage tables. (Once data is saved to the coverage tables, the icon changes to a white E on green background.) This icon appears for a patient whose eligibility has never been checked, or for one whose previous eligibility status has expired and the current eligibility request has returned new data.
![]()
White E on Red Background – Patient is not eligible but was found successfully.
![]()
White E on Orange Background – Indicates an error such as, "Patient Not Found," "Payor Unable to Respond," "Payor Nor Supported," or other errors.
![]()
Eligibility verification occurs automatically based on upcoming appointments:
Eligibility requests run in batches. You can choose how far in advance of an appointment you want eligibility checked. The default is seven days, but you can adjust the number of days to any number between the minimum of three days and the maximum of 14 days.
Note: If a patient does not have an unexpired eligibility status of Eligible, and you manually set the status to Eligible and the expiration date is in the future, that patient's eligibility will not be requested.
Same-day appointments made within the current seven-day period are checked immediately without having to wait for the next batch of requests to run.
Eligibility requests for appointments occur according to the number of days specified in the Office Manager even if the eligibility request is submitted in the month prior to the month the appointment is scheduled.
Note: You can also request eligibility checks on demand: Request Eligibility Essentials Response and Request Eligibility Pro Response. Enhanced eligibility checks are part of Eligibility Pro On Demand or the Eligibility Pro bundle. If your office is subscribed to Eligibility Essentials, and you select Request Enhanced Eligibility, you will receive a warning that a charge will be incurred if you continue.
To verify eligibility
1. In the Appointment Book or the Family File, hover your pointer over the desired eligibility indicator.
A text box appears with details applicable to the request.
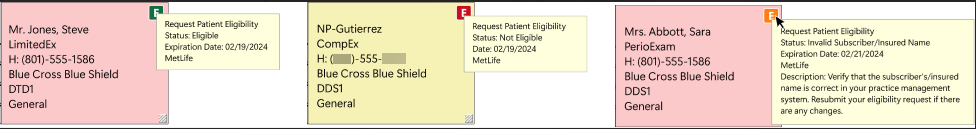
2. To request an on-demand eligibility check, click the desired eligibility icon.
A menu appears.
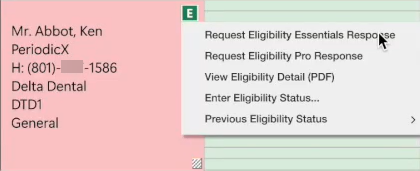
3. Click Request Eligibility Essentials Response.
The patient's insurance information is updated.